 Nondisplaced fractures of the proximal portion of metatarsals 1 through 4 can be managed acutely with a posterior splint followed by a molded, non–weight-bearing, short leg cast. Treatment of fractures distal to the tuberosity should be individualized based on the characteristics of the fracture and patient preference. Radiographs should be carefully examined to distinguish these fractures from tuberosity fractures. Proximal fifth metatarsal fractures that are distal to the tuberosity have a poorer prognosis. Avulsion fractures of the proximal fifth metatarsal tuberosity can usually be managed with a soft dressing. Stress fractures of the first to fourth metatarsal shafts typically heal well with rest alone and usually do not require immobilization. Nondisplaced fractures of the metatarsal shaft usually require only a soft dressing followed by a firm, supportive shoe and progressive weight bearing. Injuries to this ligament require referral or specific treatment based on severity. 
If the midfoot is injured, care should be taken to evaluate the Lisfranc ligament. Referral is generally indicated for intra-articular or displaced metatarsal fractures, as well as most fractures that involve the first metatarsal or multiple metatarsals. The fracture should then be characterized and treatment initiated. Initial evaluation should focus on identifying any conditions that require emergent referral, such as neurovascular compromise and open fractures. Prevention of march fractures includes stretching with gradual increments in exercise intensity and duration to avoid abrupt changes in stress. In addition, correcting predisposing biomechanical conditions such as gait training and arch supports can be beneficial.Patients with metatarsal fractures often present to primary care settings. When the patient is fully weight-bearing and pain-free with low-intensity exercise, the patient gradually increases their exercise intensity by 10% every week to avoid further stress fractures. Ī graded return to activity should be employed as a march fracture heals. 
The type of training activity, surface, and intensity can be adjusted. Shock-absorbing insoles for shoes or boots can distribute force during weight-bearing exercises. Environmental changes should be considered. Nutritional deficiencies such as low levels of vitamin D, calcium, or calories should be addressed by ensuring adequate intake and supplementation as needed. Modifiable risk factors should be treated. Additionally, a referral to an orthopedic surgeon should be placed in cases of nonunion that may need surgical fixation. Special consideration should be given to pain elicited in these areas for advanced imaging if radiographs are negative. In addition, if a fracture at these sites is present, non-weight bearing status can be achieved with crutches and casting. The exception to this treatment is areas at higher risk for nonunion, consisting of the base of the fifth metatarsal and the neck of the second metatarsal. Thus, exercise may resume with lower impact exercises such as swimming, cycling, or deep water running. Weight-bearing is allowed as long as the patient is pain-free. Immobilization is often unnecessary, and a stiff-soled orthopedic boot or walking boot may be used for 4 to 8 weeks. Acetaminophen and ice are implemented for pain and swelling. The effect of nonsteroidal anti-inflammatory drugs (NSAIDs) on fracture healing remains contested. In most cases, analgesia and rest are the only steps needed for metatarsal stress fracture healing. For example, measuring serum 25(OH), vitamin D concentration can be considered in those suspected of nutritional deficiencies. Lastly, thorough testing of the patient’s intrinsic risk factors may be needed. While bone scans are considered sensitive but not specific, MRI is both sensitive and specific for metatarsal stress fractures. Both advanced imaging modalities have been proven to be sensitive to these fractures up to 24 hours after the onset of pain. Occult, suspected fractures not visible on plain radiographs can be imaged using three-phase bone scans with technetium-99 or magnetic resonance imaging (MRI). More mature fractures may demonstrate callus formation or cortical lucency. 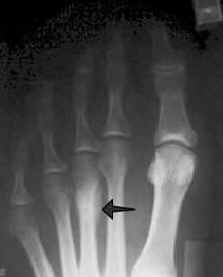
While an apparent fracture through the metatarsal may be visible on a radiograph, subtle periosteal reactions and blurring of the cortex may be the only clues of a stress fracture. However, plain radiographs have a high rate of false negatives for metatarsal stress fractures early on and may not demonstrate fractures until 2 to 4 weeks after the onset of pain. 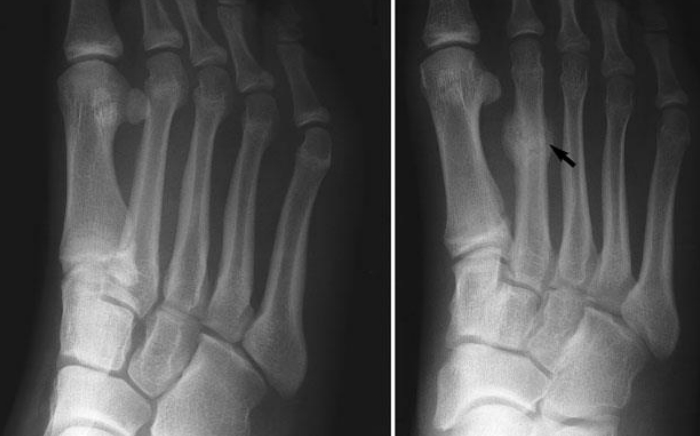
Plain radiographs are the initial imaging modality of choice. March fractures are diagnosed based on historical clues, physical examination, and confirmed with diagnostic imaging. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
